In recent years, GLP-1 medications like Ozempic, Wegovy, and Mounjaro have taken the world by storm. Originally developed to treat Type 2 Diabetes, these drugs are now being widely used for weight loss—and they’re changing the conversation around obesity almost overnight.
But are they a true medical breakthrough… or just a high-powered shortcut that doesn’t address the root of the problem?
A Medical Game-Changer—No Question
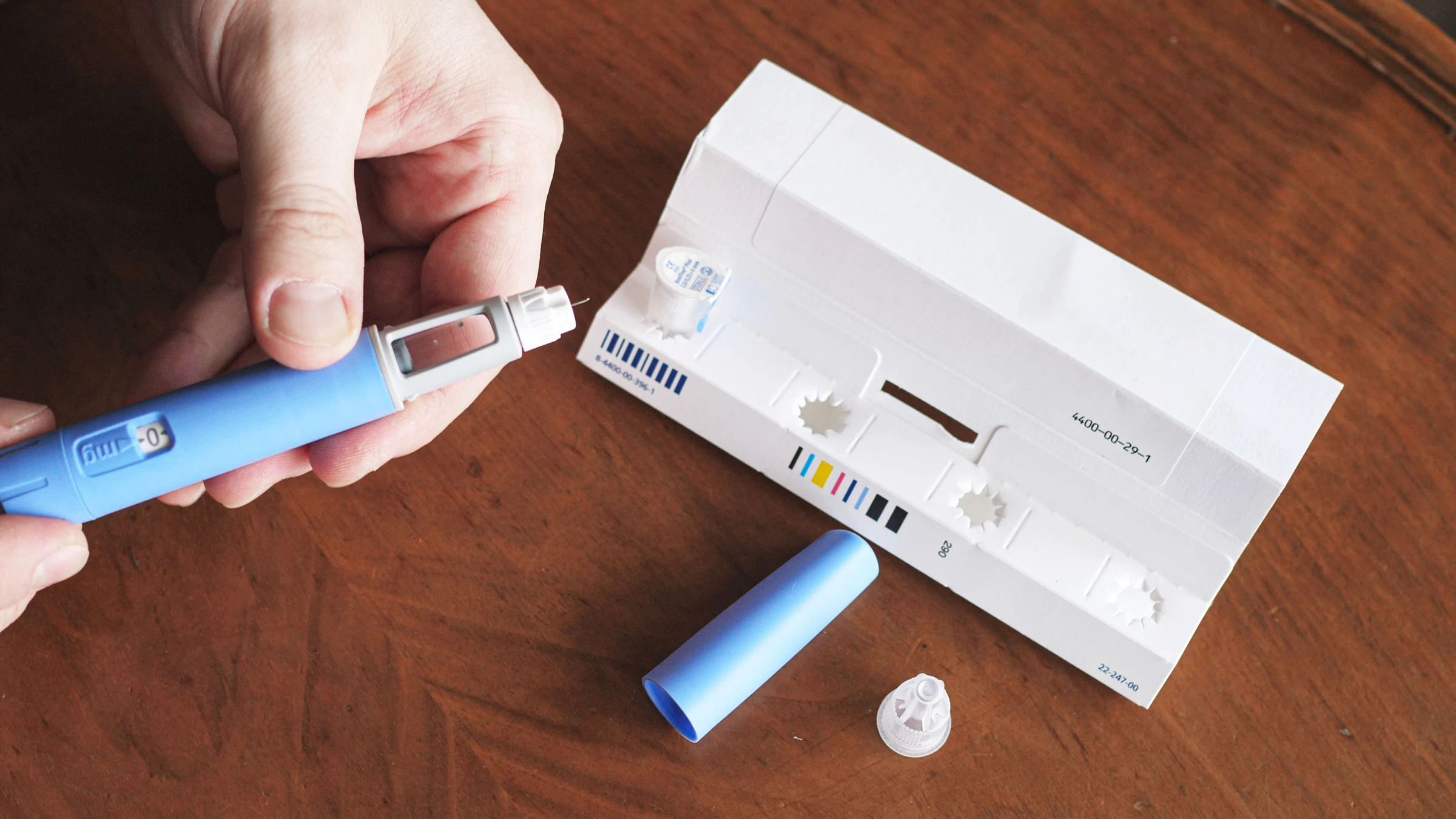

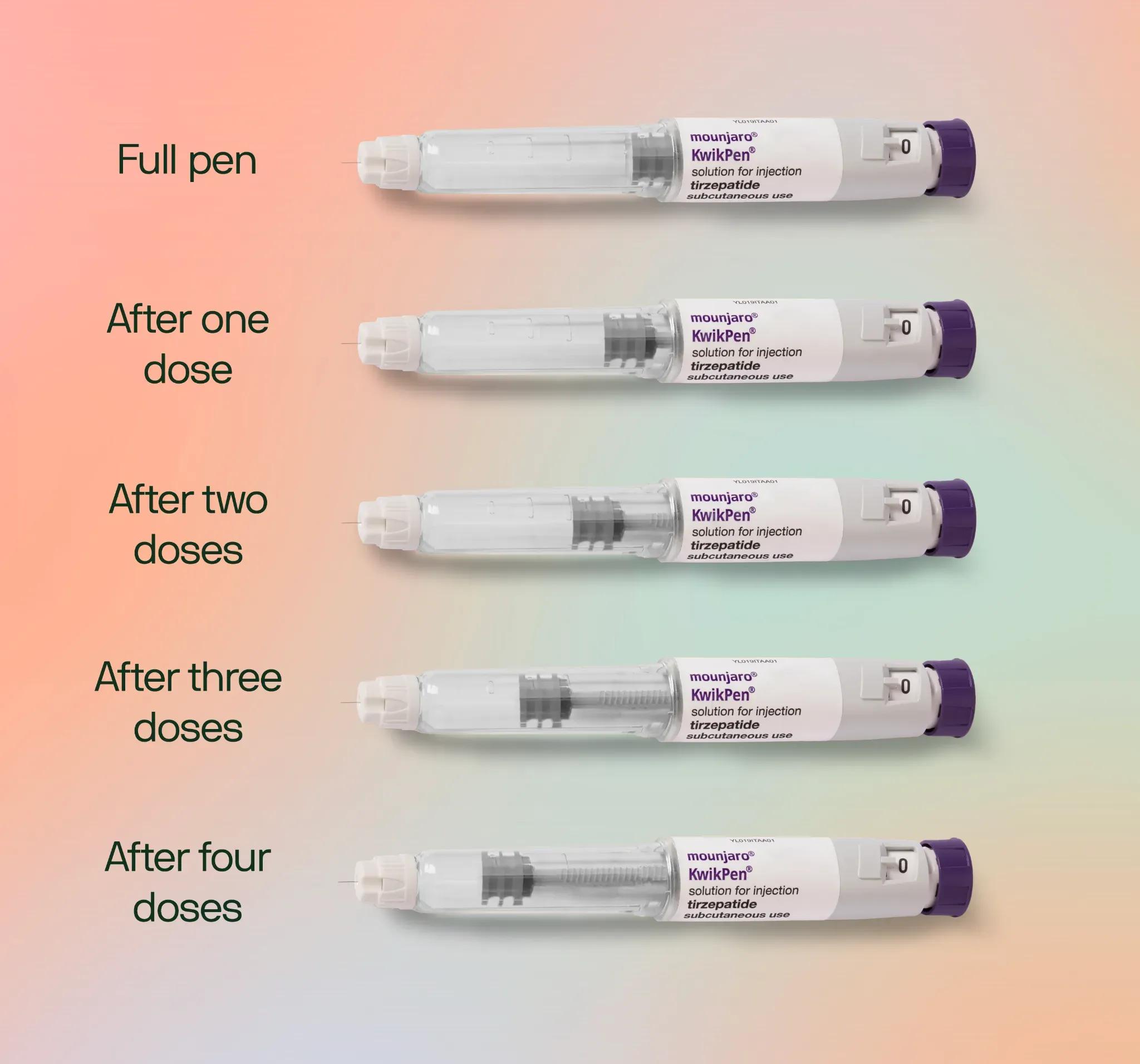
Let’s start with what’s undeniable: these medications work.
GLP-1 drugs mimic a natural hormone that regulates blood sugar, slows digestion, and reduces appetite. For many patients, this leads to significant and sustained weight loss—often far beyond what traditional diet and exercise alone have achieved.
For individuals struggling with obesity-related conditions—heart disease, diabetes, and metabolic syndrome—this isn’t cosmetic. It’s life-changing.
For the first time, millions of people who have battled weight for decades are seeing real results.
But Here’s the Hard Truth
Weight loss isn’t just about appetite—it’s about behavior, environment, and long-term habits.
GLP-1 medications reduce hunger, but they don’t teach:
- Nutritional literacy
- Emotional regulation around food
- Sustainable lifestyle habits
- Physical activity consistency
In other words, they treat the symptom (overeating), but not always the cause.
And when patients stop taking them? Many regain the weight.
That raises a tough but necessary question:
Are we solving obesity—or managing it indefinitely?
The Cultural Shift: From Discipline to Prescription




We’re also seeing a major cultural shift.
For years, weight loss was framed around discipline—sometimes unfairly so. Now, the pendulum may be swinging too far in the opposite direction, where medication becomes the default solution.
This creates a new dynamic:
- People without medical necessity seeking prescriptions
- Social pressure to use GLP-1s for appearance, not health
- A growing divide between those who can afford treatment and those who cannot
There’s also a subtle psychological impact:
If weight loss comes from a shot, does that change how we value effort, health, and self-control?
Access, Cost, and Ethics
These medications are expensive—and often not covered by insurance unless prescribed for diabetes.
That creates a two-tier system:
- Those who can afford rapid, medically-assisted weight loss
- Those who are left navigating traditional (and often less effective) methods
Meanwhile, supply shortages have impacted patients who actually need these medications for diabetes management.
This raises a broader ethical concern:
Who are these drugs really for—and who should have priority?
So What’s the Right Answer?
GLP-1 medications are not the enemy. In fact, they may be one of the most important medical advancements in metabolic health in decades.
But they are also not a complete solution.
The most responsible path forward likely looks like this:
- Use GLP-1s as a tool, not a replacement
- Combine them with nutrition education and behavior change
- Focus on long-term sustainability, not quick results
- Ensure ethical access and prioritization
Final Thought
GLP-1 medications have opened a powerful new door in healthcare.
The question isn’t whether they work—they do.
The real question is whether we will use them wisely… or rely on them in a way that avoids addressing the deeper challenges of modern health.
Because at the end of the day, lasting change doesn’t come from a prescription alone—it comes from what we build around it.